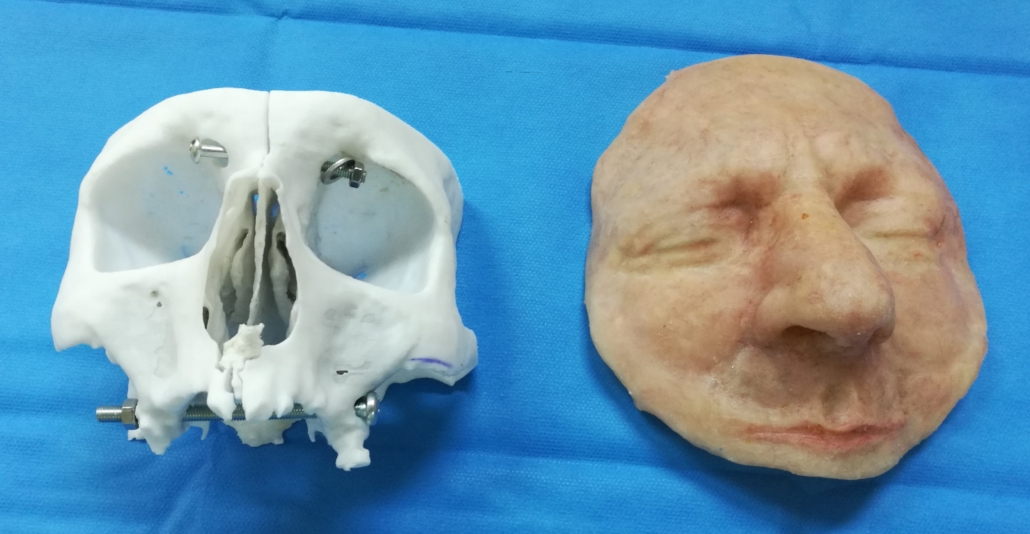
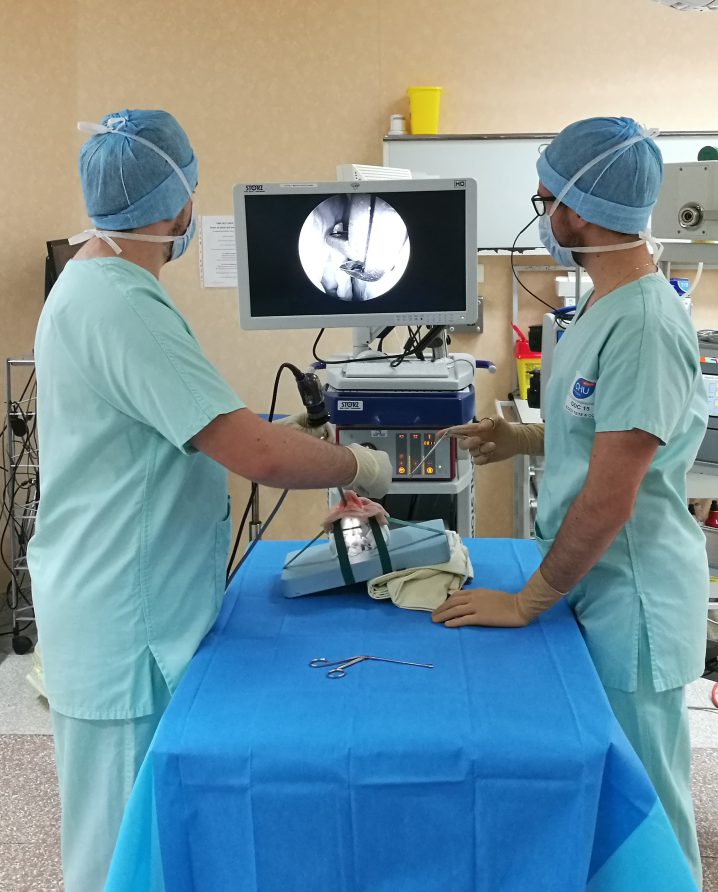
Older adults account for more than 20% of the French population (Source: INSEE 2020), yet the aging process remains poorly understood. Thanks to the simulation tools offered in this innovative workshop, participants will be able to take a leap forward in time by several years. Through this experience, they will be able to hone their skills in supporting older adults.
Why this workshop?
This workshop, offered by the School of Geriatrics and Gerontology, was designed to allow participants to experience the major impairments associated with aging.
It is led by its administrative manager, Myriam Taroudjit, and Marie-Laure Portalez, a design engineer.
Special equipment allows participants to experience firsthand the sensory challenges associated with aging. This helps them recognize the difficulties faced by older adults and better understand their behaviors and specific needs.
“A true learning-by-doing experience aimed at improving the quality of life for older adults”
The effectiveness of this simulation-based method was the subject of a study conducted by medical students at Julius-Maximilians University in Würzburg (Dr. Filz S.A., Dr. Swoboda W., et al.).
The research, conducted in the form of practical training sessions involving the use of a simulation suit, yielded the following results:
- Ability to empathize with the living conditions of older adults after the internship: 83% of participants.
- Ability to put oneself in the shoes of an elderly person after the practical training: 90% of participants.
- Understanding of an older adult’s physical condition after the practicum: 95% of participants
How?
Using simulation scenarios composed of several elements, participants put themselves in the shoes of an older adult by experiencing the physical and emotional challenges associated with aging.
Here are a few examples:
SPECIAL GLASSES
They cause altered color perception, grainy blurriness, sensitivity to glare, and/or a narrowed field of vision
HEADPHONES
It causes high-frequency hearing loss
THE WEIGHTED VEST
This vest allows participants to experience spinal curvature, anterior pelvic tilt, postural weakness, restricted mobility, loss of strength, increased physical stress, and/or impaired balance.
GLOVES
They cause reduced hand mobility, decreased dexterity, and diminished tactile sensation
ANKLE WEIGHTS
Ankle weights cause a loss of muscle strength, impaired coordination, and an unsteady gait due to shuffling
THE SOFT INSOLE OF THE OVERBOOT
This unique sole provides a cushioned feel and reduces the sensation of contact with the ground, creating a sense of instability
SPECIAL GLOVES
These other gloves enable the simulation of tremors, which are realistically reproduced through electrical muscle stimulation and a continuously adjustable control module
Feedback from our students
Every year, this innovative workshop is offered to students at the school to supplement their curriculum and deepen their understanding of older adults. The feedback has been overwhelmingly positive:
Stéphanie: “This workshop was very interesting, and everyone who works with older adults should have the opportunity to participate in this simulation workshop. Losing one’s senses is very unsettling.”

Mariam: “This afternoon, I experienced what the elderly people I care for go through every day: muscle pain, hearing and vision problems, and slowness—all caused by an environment that is no longer safe for them to navigate.”

Maïlys: “In a professional setting, I will pay even closer attention to these “pains” and how people experience and cope with them in their daily lives, so that I can best tailor my responses to their needs.”
More photos:
After winning MUSE’s Take-Off 3 competition, Drs. Herrero and Bonnel presented the PREPABLOC training program during the “Surgical Research and Innovation 2021” session at the National Academy of Surgery. The program was then awarded the prize for educational innovation! Here’s a look back at this unique training program.
PRÉPABLOC: a training program for the operating room professionals of tomorrow
Construction of the project
The launch of PREPABLOC stems from a co-creation initiative led by Dr. Herrero, with support from Dr. Ferrandis. A multidisciplinary team was assembled, comprising:
- The teaching staff at the CHU’s IBODE School,
- the Assistant Chief Residents at the CHU and ICM hospitals,
- the LIRMM teams,
- Physical therapist in the Emergency Department at the University Hospital.
Course outline
Organized and coordinated by the Innovation Accelerator, this is an innovation marathon in the form of a team competition involving groups of about ten people. Creative workshops enable participants to develop useful projects in record time and learn how to pitch them by the end of the week. The five themes were stress, communication, the future of surgical education, the appeal of operating room professions, and creating an “Escape Game.”
The future surgical nurses, who will serve as mentors to tomorrow’s surgeons, had the opportunity to participate in various theoretical and practical workshops throughout a week-long “conference.” The directors of the surgical nursing school focused their presentations on hygiene and instrumentation. The Assistant Chief Residents from the hospitals of the University Hospital and theICM , meanwhile, led theoretical courses, sharing insights into their work as hospital surgeons, conducting workshops on suturing and surgical knots, and allowing students to test their skills on a laparoscopy simulator. The LIRMM teams also collaborated at the high-tech university hospital simulation facility on the Arnaud de Villeneuve campus, which Dr. Debien and his teams operate on a daily basis. A workshop was also dedicated to casting techniques with Christophe, the lead cast technician in the CHU’s emergency department.
The objectives of this course
Train students before they begin their internship
To provide all medical students with a structured training program that is standardized before they begin their clinical rotations in surgical or emergency departments.
Reduce stress among these students
As well as that of the supervisors who welcome them into the operating rooms and who, in addition to the time required to train them on top of their regular workload, were always anxious that they might make mistakes due to a lack of familiarity in this highly controlled environment.
Raise awareness that effective teamwork is a key factor in success
This will benefit not only the patient but also foster a sense of calm in a demanding workplace.
Encourage people to pursue careers in these fields
With objective information.
Introduce students to the methodology of innovation through project-based learning at an early stage
Pso that students know how to create, structure, and present projects that align with the ambitions they may have for both their professional and academic futures.
A project supported by MUSE
This project was made possible thanks to financial support from MUSE (Montpellier University of Excellence) through a call for proposals titled “ Take OFF 3 ” won in June 2020 with the active assistance of the innovation facilitator (Dr. Christophe BONNEL and Anaïs CAUSSE). The team at MUSE’s Center for Educational Innovation (CSIP) also contributed to the project by creating an interactive, fun card game and designing an “Escape Game” that will be offered next year.
PREPABLOC: A Highly Successful Training Program
The success of the project
The creation of this Open Course Unit was a success among students. Indeed, founded by a multi-professional and multidisciplinary team, this project was particularly well-received by an interested audience composed of students in their thirdyear year of medical school, engineering students from LIRMM (robotics engineers), and IBODE students (Operating Room Nurses).
The Future of PREPABLOC
The students particularly appreciated the experience and the winning project on the future of surgical education is currently being evaluated to determine how to move forward with it. The teaching teams in Nîmes, already well-versed in these concepts, are already involved in adapting it, and the PREPABLOC team will share its experience with anyone nationwide who wishes to draw inspiration from it, in accordance with the academy’s wishes.
For the second year the Agnes McLaren Association is organizing a medical prize worth €4,000! Applications are open to students at the Montpellier-Nîmes Faculty of Medicine who will defend their clinical thesis between September 2021 and March 2023. See below for registration details and the eligibility criteria for your thesis.
This award recognizes a doctoral dissertation in medicine focusing on the health of women and/or children in precarious or vulnerable situations and funds research based on that dissertation
TheAgnes McLaren Association, founded in 2018, works to preserve the memory ofAgnes McLaren, a Scottish woman and the first female doctor to graduate from the Faculty of Medicine in Montpellier in 1878. It is in honor of this physician, who dedicated her life to caring for the most disadvantaged women or those excluded from society, that the association wishes to award a medical prize for the first time.
To mark the Faculty’s 800th anniversary in 2020, the association established the Agnès McLaren Prize in Medicine. Every two years, this prize is awarded for a clinical thesis and a post-thesis project, focusing on the health of women in precarious or vulnerable situations or the health of children exposed to precariousness and/or vulnerable situations. It also funds a project based on this thesis. The Prize, in the amount of €4,000, will be awarded in June 2023 following a preliminary selection by a committee and review by a jury composed of healthcare professionals.

In the first edition, Justine Allouche won an award for her knowledge and expertise in cervical cancer screening.
In 2021, the award was won by Justine Allouche for her work assessing knowledge and practices regarding cervical cancer screening among women in prostitution in the Gard and Hérault departments. Justine was featured in an article in Midi Libre on that occasion!
Eligibility Criteria
To be eligible for this medical award, candidates must meet several eligibility criteria:
Open to our students
Criterion 1: Be a student at the Montpellier-Nîmes School of Medicine
Year 2021-22-23
Criterion 2: Defend your thesis between September 2021 and March 2023
Thesis topic
Criterion 3: Support a dissertation whose topic addresses the health of the most disadvantaged or even marginalized women, or the health of children exposed to precariousness and/or situations of vulnerability
Post-doctoral project
Criterion 4: Thesis leading to an operational project
What are the steps to enter the contest?
The second edition of the McLaren Medical Award will take place in five phases, as follows:
by March 15, 2023
Submission of Applications
Apply online, exclusively through the Agnes McLaren Association’s website.
Pre-selection phase
Preliminary screening of the theses received by the preliminary screening committee. Five theses were shortlisted.
April 15, 2023
May 15, 2023
Selection Notice
Notification of selection sent to the five shortlisted candidates.
Final selection phase
Review of the five theses shortlisted by the jury. Candidates must submit their theses and post-thesis work by January 24, 2021.
June 2023
Sept. 2023
Award Ceremony
Presentation of the Agnes McLaren Award at the official ceremony.
We hope many of you will enter this new contest! So get writing, and good luck on your theses!
On Thursday, January 27, 2022, Dr. Catherine Alix-Panabières received the prestigious Savchuk Prize at the 15th Oncology Biennial for her work on “liquid biopsies.” A look back at 23 years of research in the field of oncology.
A career focused on the development of liquid biopsy
Dr. Alix-Panabières, director of the Rare Human Circulating Cells (CCRH) laboratory at Montpellier University Hospital, has been dedicated to her research for 23 years. Coined by her in 2010 with her German collaborator, Professor Klaus Pantel of Hamburg, the term “liquid biopsy”—which complements tissue biopsy—refers to a blood test that is performed repeatedly during a patient’s treatment.
A non-invasive procedure
A liquid biopsy provides access to circulating cells or particles released by the primary tumor or metastases. The advantage? It allows for the repeated, non-invasive monitoring of tumors located in hard-to-reach areas. After the blood sample is collected, it provides information on the tumor’s progression and, consequently, the effectiveness of treatment.
His research focuses on three key areas:
- Understanding the biology of the tumor and its prognosis.
- Technology: Dr. Alix-Panabières is working on a patent for this new technique, which enables the detection of circulating tumor cells.
- A translational clinical study. Liquid biopsy allows treatment to be tailored to each patient’s stage of disease, particularly when initiating treatment.
We extend our heartfelt congratulations to Dr. Catherine Alix-Pananières on winning this award!
In 2020, Dr. Favier and Dr. Debourdeau once again submitted a proposal to MUSE. They were selected as winners of the Take Off 4 competition, which recognizes innovations in education.
An educational innovation for safety
Physicians and surgeons are required to perform invasive procedures for the diagnosis and treatment of medical conditions. These procedures require extensive and rigorous training, which is primarily carried out during residency (beginning in the seventh year of medical school, when students begin their specialization).
The quality of medical-technical and surgical procedures must be a central focus of training, as it directly impacts patient health and safety. Technical training for medical and surgical residents must therefore include preliminary instruction to ensure the safety of patients, trainees, and supervisors alike.
Drivers of change
The use of anatomical specimens for training has been widely adopted, but this training method is limited by the availability of specimens. Another limiting factor is the difficulty in maintaining the realistic appearance of the digestive and respiratory tracts on these biological models.
The simulator as a solution
Simulator-based training helps meet safety requirements, since students do not come into direct contact with patients during their initial practice sessions, mistakes are allowed, and instructors can give students greater freedom to practice while providing educational feedback during dedicated training sessions that are more frequent because they are easier to organize. This learning method also eliminates the biological risks associated with the use of anatomical specimens.
The specific areas involved
Since simulation is a very expensive and time-consuming process to set up, Drs. Favier and Debourdeau conducted preliminary studies to determine in which areas it could be most useful.
According to their research, simulation-based training is necessary for the following procedures:
- Diagnostic and Interventional Esophagogastroduodenoscopy (Gastroenterology)
- Diagnostic and Interventional Colonoscopy (Gastroenterology)
- Endoscopic surgery of the nose, sinuses, and anterior skull base (ENT, neurosurgery, maxillofacial surgery)
- Flexible endoscopy for the diagnosis of the upper aerodigestive tract (ENT, anesthesiology and critical care, oncology)
- Rigid bronchoscopy (ENT specialists, pediatricians, pulmonologists)
Proven effectiveness
These procedural simulators have been scientifically validated for initial training and have proven their effectiveness. In total, these programs involve 220 residents in the Montpellier-Nîmes area (20 gastroenterologists, 18 ENT specialists, 6 neurosurgeons, 6 maxillofacial surgeons, 15 pulmonologists, 125 anesthesiologists and intensivists, and 20 oncologists).
A project that builds on the previous one
Remember, we previously mentioned, in one of our articles, Drs. Favier and Debourdeau, who were winners of a previous MUSE Take Off competition. That project involved the development of an app called SPART APP, designed to assess the technical skills of medical residents.
This project builds on the work of Spart-APP. In fact, this app, which can track residents’ technical progress, could eventually be integrated with a simulation platform. This platform will enhance real-time learning for students who are struggling, through an active and dynamic teaching approach.
In 2020, Dr. Valentin FAVIER, in collaboration with Dr. Antoine Debourdeau, once again submitted a proposal to the MUSE call for projects, which aims to support the pedagogical transformation of educational programs. His project, titled “Application for Monitoring Learning Progress and the Execution of Technical Procedures in Medicine,” was selected as a winner.
The origins of the project
The quality of medical training is a public health issue that is essential to provide the population as effectively as possible for years to come. Medical competence takes a long time to acquire, during which students must master theoretical and technical skills. Medical residents must learn the skills and procedures that will form the foundation of their medical practice during the 4 to 6 years of their residency. Their theoretical knowledge is frequently assessed through written exams.
Currently, medical residents complete their clinical rotations according to a predefined educational curriculum, divided into semesters, and receive their residency degree upon completion of their program after defending a thesis.
Nevertheless, during their residency, medical students work full-time at the hospital, and their university-based training on campus is reduced to just a few days a year.
However, the medical curriculum does not take into account the technical skills of medical residents, and there are few tools available to track their acquisition and monitor the learner’s progress throughout their rotations.
It was against this backdrop that Drs. Favier and Debourdeau decided to develop an app to track the progress of healthcare students in terms of their technical skills.

The Birth of SPART APP
SPART-App is a project that aims to provide medical residents, their trainers, and the educational coordinator with a mobile app to record every procedure performed throughout their residency (e-logbook). This pilot project covers the specialties of anesthesiology and critical care, gastroenterology, otolaryngology, and maxillofacial surgery. Here are its objectives:
For the learnerFor the learner, this digital notebook will allow them to track their progress in real time (success rate, learning curve), identify areas for improvement, and alert their instructor if their practice is insufficient.
For the instructor, this tool will help identify the challenges faced by the learner, clarify and find solutions to roadblocks, and facilitate a debriefing.
For the academic supervisor, it will enable them to tailor educational objectives on a case-by-case basis according to the challenges students face, identify training gaps (particularly in the number of procedures performed) so that supervisors can be alerted, and propose concrete, personalized solutions to the student and their supervising team.

The app: a strategic choice
The digital, via an app that can operate offline, eliminates the need for procedure logs that are not regularly updated. The resident will be able to evaluate their procedure immediately after performing it, on their smartphone.
Each resident will be provided with a student account specific to their specialty. In this account, the resident can record every procedure performed over time, detailing the procedure itself, whether it was successful or unsuccessful, and any difficulties encountered. Using the data entered into the application, it is possible to track their learning curve.
The supervisor of the procedure may, if they wish, approve the intern’s assessment of the procedure and use it as a basis for a technical debriefing . The instructor will have access to the data for each of the residents they supervise. This will allow the head of education (department head) to ensure that each resident performs a sufficient number of procedures and to identify residents who are struggling so they can provide them with additional support.
The Impact of START APP
Through this project, Dr. Favier hopes to advance the development of technical skills and generate short-, medium-, and long-term impacts.
In the short term, SPART-app will provide an overview of the current state of technical training in medicine and surgery. At present, this training is subjective and varies depending on the instructors. This project would serve as a tool to standardize and streamline the monitoring of students.
In the medium term, this program will enable students to track their progress and tailor their course of study based on their areas of weakness and strengths. The project could also be expanded to include programs other than those mentioned above. This educational innovation could then be rolled out nationwide under the leadership of the University of Montpellier.
From a scientific perspective, the data collected through this app will be used to conduct educational studies in each of the relevant specialties, with the aim of evaluating the impact of interventions (including simulation, a component also studied by Dr. Favier) on the acquisition of technical skills to guide changes in teaching practices in a rational manner.
In the long term,this educational transformation will lead to improved practices at the local and national levels, with a tangible impact on enhancing patient safety by reducing the risk of technical errors.
Currently, the project led by Dr. Favier and Dr. Debourdeau is moving forward and is expected to be launched soon.
In 2018, Dr. Valentin FAVIER submitted a proposal to the MUSE call for projects, which aims to support educational reform in training programs. His project, titled “Learning Anatomy and Surgery Through Simulation and 3D Printing,” was selected as a winner.
MUSE “Take-Off”—what is it?
The MUSE project “ Montpellier University of Excellence brings together 16 institutions toward a shared goal: to establish in Montpellier a research-intensive, thematically focused university, internationally recognized for its impact in fields related to agriculture, the environment, and health, capable of becoming, for all members of the consortium, a close academic partner with which they will be strongly connected and of which they can be proud.
Through these “Take Off” calls for proposals, it supports the educational transformation strategy of the institutions and components of the MUSE consortium. Over the past three years, I-SITE MUSE has raised €6 million to support educational innovations through this program. The “Learning Anatomy and Surgery through Simulation and 3D Printing” project is one of the projects selected for Take-Off #1. Learn more about it in this article!

Enhancing Learning Through Simulation: Dr. Favier’s Challenge
Healthcare simulation is a key focus of medical education in the 21st century. To improve the safety of clinical practice and education, the French National Authority for Health (HAS) released a report in 2012 outlining the prospects for the development of healthcare simulation in France.
So what exactly are surgical simulators?
Surgical simulators are educational tools that are an integral part of this concept. They enable the training of young surgeons, helping them to familiarize themselves with surgical equipment, anatomy, and surgical techniques, but they are also useful throughout continuing medical education for refresher training. Another major benefit lies in the ability to develop new surgical techniques, allowing more experienced surgeons to perform innovative approaches or test new instruments.
The project's objectives
The project is intended for surgical residents, who will have the opportunity to practice on these simulators. The work currently underway is now focused on several objectives:
Improving the segmentation of bone structures and pathological processes from CT images to generate 3D objects.
Improving the biomechanical characterization of human skull base bone using innovative mechanical tests designed specifically for this purpose. A better understanding of biomechanics will enhance the realism of the materials used in simulation.
Conduct large-scale simulator testing with the target audience (ENT surgery residents) using the simulation facility at the School of Medicine, in collaboration with the Nancy-Lorraine School of Surgery.
A project made possible by MUSE
As the winner of the project, Dr. FAVIER received a €10,000 grant from MUSE. This grant was used to advance his project on surgical simulators. Specifically, it was used to:
- Compensation for a Master’s 2 intern in computer science for research and algorithm development to implement the simulation.
- Perform mechanical testing of the simulation platform.
- The purchase of materials needed to conduct the simulation and produce 3D prints.
“The The Avicenne Multidisciplinary University Health Center (MSPU) was inaugurated in Cabestany near Perpignan in 2018. In June 2021, two additional MSPUs were added to this regional network. To mark this opening, a formal ceremony was held on Thursday May 27 to review the Cabestany MSPU and present the plans for the two new MSPUs.”
MSPU: What is it?
A Multidisciplinary Health Center is a multidisciplinary health center that has entered into an agreement with the Regional Health Agency (ARS) and a university with a medical program to promote training and research in primary care.
Avicenne's MSPU: A Positive Outcome
This MSPU, led by Dr. Mark OUDE ENGBERIK and comprising some thirty healthcare professionals from various fields, has carried out several projects over the past five years. Two major projects were discussed at this conference:
- The TSAPPproject, which aims to train healthcare professionals on providing access to care for people with disabilities.
- The SPES (Primary Care, Environment, and Health) project, which aims to promote health and environmental awareness among healthcare professionals and the general public.
In terms of academic training, this MSPU has 16 clinical instructors in various fields of healthcare and takes on 6 to 10 interns each year.
Two new MSPUs in the region
Following the success of the projects carried out by the Avicenne MSPU, two additional centers were opened in the region to meet local needs in this area.
MSPU LA SOURCE
- Opened in February 2020, this primary care clinic is located in Vergèze and is managed by Dr. Céline Varraut.
- It has a staff of 25 professionals across 10 different healthcare fields
- Its objectives focus on three main areas: the region, training, and healthcare
MSPU Pauline Lataud
- This primary care practice operates across multiple locations, with offices in Castries, Prades-le-Lez, Saint-Georges-d’Orques, and Vendargues, and is managed by Dr. Philippe Lognos.
- It has a staff of 50 professionals across nine different healthcare fields
- It also focuses its objectives on the same themes as the previous one.
A joint initiative is taking shape around these three MSPUs: to build a research network and make the service accessible to local residents.
Downtown Montpellier: Historic Building
2 rue École de Médecine
CS 59001
34060 Montpellier cx 2
04 34 43 36 00
North Montpellier
641 Avenue du Doyen Gaston Giraud
34070 Montpellier
04 34 43 35 00/01
Nîmes
186 Chemin du Carreau de Lanes
CS 83021
30908 Nîmes Cedex 2
04 66 02 81 81
Montpellier Botanical Garden
34000 Montpellier